Source: Health and environment — EEA
The quality of Europe’s drinking and bathing water have improved but air and noise pollution continue to cause serious health impacts. About 460 000 premature deaths were attributed to fine particulate matter in 2011. Further reductions in pressures may be offset by changing exposure patterns and vulnerabilities, linked to trends such as climate change, urbanisation and population ageing. This points to the need for more integrated approaches to addressing social, economic and environmental determinants of health.
Context
Good quality natural environments provide multiple benefits to health and well-being [1]. In contrast, air pollution, noise, poor quality water, chemicals, radiation, and environmental degradation cause diverse impacts on human health.
Understanding of the links between the environment and human health has evolved from perceiving them as isolated issues towards recognising the interdependencies between complex systems. Large-scale challenges such as climate change and biodiversity loss can have potentially wide-ranging, long-term, and irreversible effects on human health and well-being. Such challenges call for an approach that takes account of the linkages between human and animal health, environmental drivers, and the socio-ecological context of disease emergence [1] [2] [3]
Europe’s long-term policy increasingly adopts a more systemic perspective that links the environment, human health and well-being. The Roadmap to a Resource Efficient Europe, for example, includes targets on natural resources that provide for basic human needs [4]. Promoting good health and reducing inequalities is also an integral part of the EU’s Europe 2020 growth strategy [5] [6] [7]
One of the three thematic priority objectives set out in the EU’s 7th Environment Action Programme is ‘to safeguard citizens from environment-related pressures and risks to health and well-being’ [8]. At the global level, the World Health Organization (WHO) and related United Nations (UN) processes address a range of environmental and climate-related challenges to health and well-being [9] [10] [11] [12] [13]
Trends
Knowledge gaps, uncertainties and shortages of data limit understanding of the complex interactions between human health, multiple environmental pressures, and social and demographic factors. This section focuses on some specific themes for which the EEA gathers information and has an assessment role, including air pollution, noise, and water quality. It concludes with a brief discussion of more systemic issues.
Air pollution
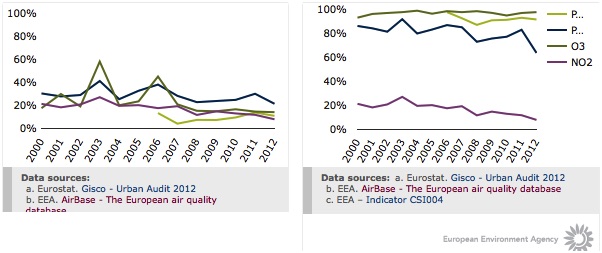
Air pollution remains a major environmental health risk in Europe, contributing to the burden of respiratory and cardiovascular diseases, lung cancer, and other health effects [14] [15] [16]. Despite improvements with respect to some pollutants, exposures to particulate matter, ozone and carcinogenic benzo(a)pyrene are of high concern. This is particularly evident using the estimates based on WHO air quality guidelines [15], which are more stringent than EU air quality standards [17] (Figure 1)
In 2011, an estimated 458 000 premature deaths in 40 European countries were attributed to fine particulate matter [18]. There are no estimates of less severe but more widespread impacts of air pollution, such as use of medication or hospitalisations. Ambient air pollution, combustion processes, energy efficiency measures in buildings, consumer products, and human behaviour all affect the quality of indoor air. Since European citizens spend more than 90% of time indoors, coordinated efforts are needed to prevent the potential health effects of exposure to indoor air pollution [19]
Water quality
Progress in collecting and treating wastewater in the EU since the 1990s has contributed to a sizable improvement in bathing water quality (Figure 2), and reduced public health risks in parts of Europe [20]
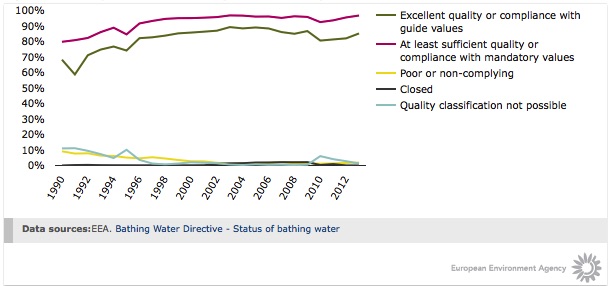
However, chemical pollutants, eutrophication, and harmful algal blooms continue to affect the quality of surface, ground, and marine waters [21] [22], potentially impacting human health. Water scarcity is also an emerging challenge. And both the quality and the quantity of water resources can be affected by climate change [1] [23]
Noise
Environmental noise is a source of annoyance and has been linked to increased risk of cardiovascular diseases [24] [25]. It is estimated that at least 125 million people in Europe were exposed to high levels of road traffic noise in 2011. And exposure to environmental noise has been estimated to contribute around 10 000 cases of premature deaths due to coronary heart disease and stroke each year, with almost 90% of the noise-related health impacts being associated with road traffic noise [26]
Chemicals
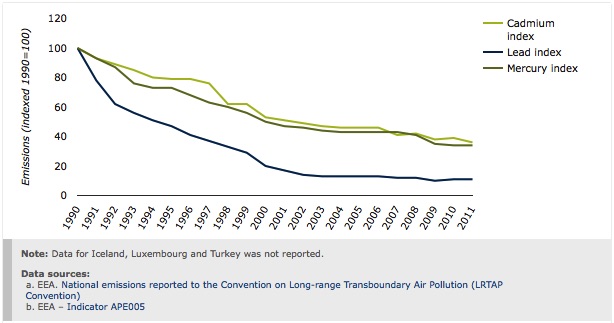
European policy has been effective in addressing emissions and ambient concentrations of certain chemicals [27] (Figure 3), and horizontal chemical legislation (REACH) [28] aims to better protect the environment and human health. Persistent, bioaccumulative, and toxic chemicals are of particular concern, as are substances that can affect the hormonal system (endocrine disruptors) [1] [29] [30]. The risks associated with pharmaceuticals in the environment, including antimicrobial resistance and endocrine disruption in wildlife and people, are increasingly recognised, with implications for precautionary action and wastewater treatment [1] [29] [31] [50]
Further efforts are needed to assess the health impacts of exposure to multiple chemicals from different sources, especially in vulnerable groups such as children. Current activities to streamline existing information on chemicals in the environment, including human biomonitoring data, should improve the knowledge base [32]
Systemic issues
There is a growing recognition that major public health issues, such as cardiovascular and respiratory diseases, cancer, and obesity, result from the interplay of multiple factors, including environmental pressures [1] [33] [34] [35]. The European population’s vulnerability and ability to adapt to environmental pressures depends on a variety of long-term trends.
For example, the population age structure shapes vulnerability to health risks. Although EU-28 average life expectancy at birth exceeds 80 years, the expected years lived without disability are below 62 years for both men and women [36]. The proportion of people aged 65 and over (EU-27) is projected to increase from 18% in 2011 to 30% by 2060 [37] [38], further shifting disease burdens and increasing the contribution of disabilities [39]
Another important trend is urbanisation. The proportion of Europe’s population living in urban areas increased from 51% in 1950 to 73% in 2011, and is projected to reach 82% in 2050 [40]. Environmental impacts on health and well-being may be particularly pronounced in urban settings, where multiple pressures coexist and affect large populations. Contrastingly, well planned urban areas that afford access to natural environments can deliver health and well-being benefits [1]. The EU Green Infrastructure Strategy [41] and improved spatial analysis can contribute to better urban development and spatial planning. Potential climate change impacts in urban systems also point to a need for dedicated adaptation measures [42]
Health and well-being impacts of climate change are related mainly to extreme weather events and changes in the distribution of climate-sensitive diseases. Some regions and population groups in Europe are particularly vulnerable to these threats [43] [44]. A very likely increase in the frequency and intensity of heat waves, particularly in southern Europe, is projected to increase heat-related deaths unless adaptation measures are implemented [44][45]. Heavy precipitation and flooding can have profound effects on mental health and welfare [46]. Anticipated climate change impacts on some diseases, including those transmitted by mosquitoes and ticks, highlight the need to improve response mechanisms [47][48][49]
Prospects
Human health and well-being concerns are powerful drivers for environmental policy, but they are at present addressed in a dispersed way. Implementation of existing policies is likely to further reduce specific burdens, but broader and more integrated approaches to addressing social, economic, and environmental determinants of health are needed [1]
Widening the policy focus to domains such as consumption and production, resource efficiency, natural capital, ecosystem services, and spatial planning would require a stronger multidisciplinary and multi-stakeholder dialogue to account for values and attitudes. Decision-making also needs a precautionary approach, which acknowledges uncertainties, especially for emerging issues such as nanotechnology [50]
Human health and well‑being ultimately depend on well‑functioning ecosystems and the way we use natural resources [9]. The synergies and trade-offs resulting from close interdependencies between the core resources, such as food, water, energy and other materials indirectly affect human health and well‑being, often through impacts on the environment [51]. In addition, the role of large-scale ecological and societal transitions for population health and well-being is increasingly recognised, influencing both health effects and the possibilities for public interventions to achieve a more sustainable society [52]
References
[1] EEA/JRC (2013), Environment and human health, EEA Report No 5/2013, European Environment Agency and the European Commission's Joint Research Centre. [2] EEA (2010), The European environment — state and outlook 2010: Synthesis, State of the environment report, 1/2010, European Environment Agency, Copenhagen. [3] EEA-Eionet (2013), 'Foresighted reasoning on environmental stressors and health', European Environment Agency. [4] EC (2011), Communication from the Commission to the European Parliament, the Council, the European Economic and Social Committee and the Committee of the Regions 'Roadmap to a Resource Efficient Europe', COM(2011) 571 final of 20 September 2011. [5] EC (2010), Communication from the Commission 'Europe 2020 — A strategy for smart, sustainable and inclusive growth', COM(2010) 2020 final of 3 September 2010. [6] EC (2007), White paper — Together for health: a strategic approach for the EU 2008–2013, COM/2007/0630 final. [7] EU (2014), Regulation No 282/2014 of the European Parliament and of the Council of 11 March 2014 on the establishment of a third Programme for the Union's action in the field of health (2014–2020) and repealing Decision No 1350/2007/EC. [8] EU (2013), Decision No 1386/2013/EU of the European Parliament and of the Council of 20 November 2013 on a General Union Environment Action Programme to 2020 Living well, within the limits of our planet, OJ L 354, 20.12.2013, pp. 171–200. [9] MA (2005), 'Millennium Ecosystem Assessment — Ecosystems and human well‑being: health — synthesis report', Island Press, New York, USA. [10] UN (2012), General Assembly resolution 66/288: The future we want, A /RES/66/28, 11 September 2012, United Nations. [11] UNEP (2014), Synergies among the Basel, Rotterdam and Stockholm Conventions, accessed 14 March 2014. [12] WHO, (2010), Parma Declaration on Environment and Health. Fifth Ministerial Conference on Environment and Health 'Protecting children's health in a changing environment' Parma, Italy, 10–12 March 2010, World Health Organization Regional Office for Europe, Copenhagen, Denmark. [13] WHO (2013), 'Health 2020: a European policy framework supporting action across government and society for health and well-being', World Health Organization Regional Office for Europe, Copenhagen, Denmark. [14] WHO (2006), 'Air quality guidelines for particulate matter, ozone, nitrogen dioxide and sulfur dioxide. Global update 2005. Summary of risk assessment', World Health Organization, Geneva, Switzerland. [15] WHO (2013), 'Review of evidence on health aspects of air pollution — REVIHAAP project technical report', World Health Organization, Regional Office for Europe, Copenhagen, Denmark. [16] IARC (2013), Outdoor air pollution a leading environmental cause of cancer deaths, Press Release No 221, 17 October 2013, International Agency for Research on Cancer, World Health Organization, Lyon, France. [17] EEA (2013), Air quality in Europe — 2013 report, EEA Report No 9/2013, European Environment Agency, Copenhagen, Denmark. [18] EEA (2014), Air quality in Europe — 2014 report, EEA Report No 5/2014, European Environment Agency, Copenhagen, Denmark. [19] SCHER (2007), 'Opinion on risk assessment on indoor air quality', Scientific Committee on Health and Environmental Risks, European Commission. [20] EEA (2014), European bathing water quality in 2013, EEA Report No 1/2014, European Environment Agency, Copenhagen, Denmark. [21] EEA (2011), Hazardous substances in Europe's fresh and marine waters — An overview, Technical report No 8/2011, European Environment Agency, Copenhagen, Denmark. [22] ETC/ICM (2013), Hazardous substances in European waters — Analysis of the data on hazardous substances in groundwater, rivers, transitional, coastal and marine waters reported to the EEA from 1998 to 2010, Technical Report, 1/2013, Prague. [23] EEA (2012), Towards efficient use of water resources in Europe, EEA Report No 1/2012, European Environment Agency, Copenhagen. [24] WHO (2009), 'Night noise guidelines for Europe', World Health Organization, Regional Office for Europe, Copenhagen, Denmark. [25] JRC (2013), Final report ENNAH — European Network on Noise and Health, Scientific and Policy Report by the Joint Research Centre of the European Commission. [26] EEA (2014), Noise in Europe 2014, EEA Report No 10/2014, European Environment Agency, Copenhagen, Denmark. [27] EEA (2015), Heavy metal (HM) emissions (APE 005). [28] EU (2006), Regulation (EC) No 1907/2006 of the European Parliament and of the Council of 18 December 2006 concerning the Registration, Evaluation, Authorisation and Restriction of Chemicals (REACH), OJ L 396, 30.12.2006, pp. 1–849. [29] EEA (2012), 'The impacts of endocrine disrupters on wildlife, people and their environments — The Weybridge+15 (1996–2011) report', Technical report No 2/2012, European Environment Agency, Copenhagen, Denmark. [30] WHO/UNEP (2013), 'State of the science of endocrine disrupting chemicals — 2012', World Health Organization, United Nations Environment programme, Geneva, Switzerland. [31] WHO (2014), 'Antimicrobial resistance — global report on surveillance', World Health Organization, Geneva, Switzerland. [32] EC (2012), Communications from the Commission to the Council: The combination effects of chemicals — Chemical mixtures, COM(2012) 252 final, Brussels 31.5.2012. [33] Balbus, J. M., Barouki, R., Birnbaum, L. S., Etzel, R. A., Gluckman, S. P. D., Grandjean, P., Hancock, C., Hanson, M. A., Heindel, J. J., Hoffman, K., Jensen, G. K., Keeling, A., Neira, M., Rabadan-Diehl, C., Ralston, J. and Tang, K.-C. (2013), Early-life prevention of non-communicable diseases,Lancet381(9860), accessed 30 May 2014. [34] Vineis, P., Stringhini, S. and Porta, M. (2014), 'The environmental roots of non-communicable diseases (NCDs) and the epigenetic impacts of globalization', Environmental research. [35] WHO (2011), 'Global status report on noncommunicable diseases 2010', World Health Organization, Geneva, Switzerland. [36] EC (2014), European Community Health Indicators (ECHI), accessed 14 March 2014. [37] Eurostat (2014), Population structure and ageing, accessed 14 March 2014. [38] EEA (2014), Assessment of global megatrends — an update, European Environment Agency, accessed 9 July 2014. [39] IHME (2013), The global burden of disease: generating evidence, guiding policy – European Union and European Free Trade Association regional edition, Institute for Health Metrics and Evaluation, Seattle, WA. [40] UN (2012), World urbanization prospects — The 2011 revision, ESA/P/WP/224, United Nations Department of Economic and Social Affairs. [41] EC (2013), Communication from the Commission to the European Parliament, the Council, the European Economic and Social Committee and the Committee of the Regions: Green infrastructure — enhancing europe's natural capital, COM/2013/0249 final. [42] EEA (2012), Urban adaptation to climate change in Europe, EEA Report No 2/2012, European Environment Agency, Copenhagen, Denmark. [43] EEA (2012), Climate change, impacts and vulnerability in Europe 2012 — an indicator-based report, EEA Report No 12/2012, European Environment Agency, Copenhagen, Denmark. [44] IPCC (2014), Climate change 2014: Impacts, adaptation and vulnerability, Cambridge University Press, Cambridge, United Kingdom, and New York, USA. [45] WHO (2011), Climate change, extreme weather events and public health, meeting report, 29–30 November 2010, Bonn, Germany, World Health Organization, Regional Office for Europe, Copenhagen, Denmark. [46] WHO and PHE (2013), Floods in the WHO European Region: health effects and their prevention, World Health Organization Regional Office for Europe and Public Health England. [47] Suk, J. E. and Semenza, J. C. (2011), 'Future infectious disease threats to Europe',American Journal of Public Health 101(11), pp. 2 068–2 079. [48] Lindgren, E., Andersson, Y., Suk, J. E., Sudre, B. and Semenza, J. C. (2012), 'Monitoring EU emerging infectious disease risk due to climate change', Science336(6080), pp. 418–419. [49] ECDC (2012), Assessing the potential impacts of climate change on food- and waterborne diseases in Europe, Technical Report, European Centre for Disease Prevention and Control, Stockholm, Sweden. [50] EEA (2013), Late lessons from early warnings: science, precaution, innovation, EEA Report No 1/2013, European Environment Agency, Copenhagen, Denmark. [51] EEA (2013), Environmental indicator report 2013 – natural resources and human well-being in a green economy, European Environment Agency, Copenhagen, Denmark. [52] Rayner, G. and Lang, T. (2013), 'Ecological public health: reshaping the conditions for good health', Routledge, New York.


 Aragonese
Aragonese English
English Spanish
Spanish